At the McDonough School of Business, professor Peter Jaworski teaches students how to apply ethics to the business world.
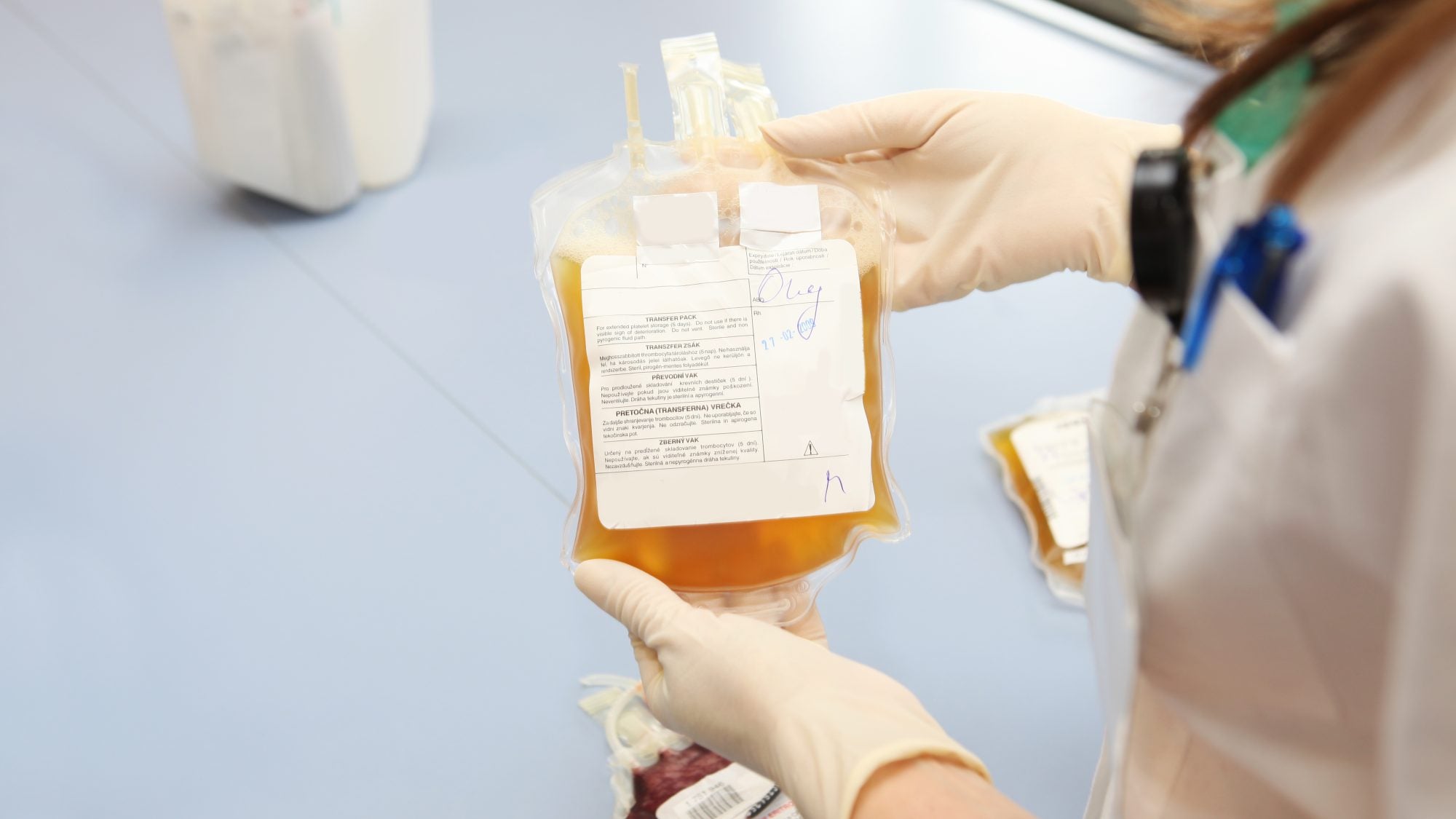
Outside of class, he applies ethics to an entirely different world: blood. Specifically, plasma — the yellow, watery part of blood that ferries vital proteins, nutrients and electrolytes around the body.
For a decade now, Jaworski has tackled the thorny ethics and economics of global plasma collection, a multibillion-dollar business that supplies life-saving plasma-based medications to patients around the world.
“I’m known as the guy who talks about plasma,” said the business professor, whose X handle is the Plasma Professor.
Plasma-based medications are used to treat patients with immune disorders and deficiencies, hemophilia, neurological disorders, rare diseases, and those experiencing burn injuries or trauma, among other uses. A lot of plasma is needed: It takes 130 plasma donations to treat one person with an immunodeficiency for one year, according to the Department of Health and Human Services.
The demand for plasma-based therapies is growing, particularly as more rare diseases are diagnosed, and that demand relies on donors. Most countries don’t collect enough plasma to meet patient needs, including Australia, France, Italy and Jaworski’s home country of Canada, he said.
The majority of countries — with the exception of the United States, Austria, Germany, Hungary, Uzbekistan, Ukraine and the Czech Republic — ban paying donors for their plasma.
For Jaworski, there’s an obvious fix: compensating donors.
“Usually I ask my students, can you guess the country that contributes the most plasma in the world for these medicines that are made from plasma? America with just 5% of the global population provides 68% of the plasma used to manufacture lifesaving medicines for the whole world. That includes the high-income countries that ban payment. All of them rely on plasma donated in the U.S.,” he said.
“Everybody in a way either directly or indirectly uses the system where we compensate donors. So then why don’t we expand it to other countries? That’s where my head is at.”
Jaworski has collected data on how much plasma every country collects, written papers on the ethics of compensation and helped repeal international policies banning donor compensation. First in Alberta, Canada, in 2020. And soon, he hopes, in Greece.

This project may have started as a rabbit hole, but now, it’s his life’s passion.
“I’ve met so many patients who rely on medicines made from plasma,” he said. “We don’t have enough of this medicine. There are people who have no access to it. When you get that really personal story, it feels like you’ve got to do something about it. How can you not?”
The Economics of Plasma Collection
Jaworski discovered the world of plasma collection by chance, through a student.
Back in 2016, Doug Grant (MBA’16), founder of Atlantic Fish Company, had co-founded a start-up called Hemeos, which would pay individuals to donate bone marrow. When the Department of Health & Human Services proposed banning compensation for bone marrow donors, jeopardizing his new venture, Grant asked his professor for help.
Jaworski dove into the topic and wrote a letter signed by ethicists and economists, which he presented before the department. It worked.
“It felt like the letter made a difference, and that felt like the most meaningful thing I had ever done in my life,” he said.
In his research, Jaworski found a corollary in plasma donations. Many of the same objections to paying people for bone marrow applied to plasma.

Jaworski started collecting data on how much plasma every country collects. As of December 2025, he totaled 1,247 blood plasma donation centers in the United States. In comparison, Denmark has three collection centers; Italy, 13.
Americans’ donations make up 68% of global plasma collections manufactured for medicine. France, which bans compensation, came up 1.5 million liters short on their plasma collection needs in 2024, according to his data.
“Not one of them can figure out a way to collect enough plasma,” he said. “We have overwhelming evidence that paying people is effective. You either pay people directly, allowing it within your country, or you pay Americans, but you’re paying donors.
“If 10% of the world population had the option with donor compensation, then I think patients would breathe a lot easier.”
Ethical Concerns
Jaworski, who has a master’s in philosophy and public policy from the London School of Economics and a Ph.D. in philosophy from Bowling Green State University, applies his ethics background to this work. In writing papers on the ethics of donor compensation, he’s learned most countries ban payment for moral reasons.
Some raise ethical concerns that the compensation system could exploit vulnerable people and commodify donors. In a 2021 study, researchers found that most plasma donors in the United States are often low-income and younger.
Others raise concerns about donor safety or whether paying donors undermines opportunities or motivations for altruism. In his work, Jaworski addresses each of these.
“The exploitation concern is often an apples-to-oranges comparison,” Jaworski said. “People say that the companies make billions, while donors get $50. That seems unfair. But that compares an aggregate to an individual donor. For an apples-to-apples comparison, you need to look at it unit-to-unit or aggregate to aggregate.”
He noted that per liter of plasma, the collecting company makes an average of $15 to $20 in pre-tax profit, while the donor makes an average of $60-$70. He also noted that U.S. donors received $4.7 billion in donor fees in 2025, while the companies made $4.5 to $5 billion in pre-tax profits from the medicines they made using U.S. plasma.
“The point of plasma collection is to collect enough to meet the needs of patients. It’s not to give you or me an opportunity to express our altruism. It’s not to stitch us together in community. It’s not to give gifts. It’s more important that we have enough to save lives,” he said.
“People say, ‘In America, they have to pay people to donate blood and plasma. But in New Zealand or Australia, we do it just for cookies and milk.’ I come along and say, ‘Well, those cookies and milk are good enough for 44% of the plasma that you need. The rest – more than half – comes from the Americans who get paid for their plasma.’”
Jaworski has also partnered with Assistant Professor Bill English to address economic concerns on the effects of blood plasma compensation on blood donations.
Does paying people for plasma have an adverse impact on unpaid blood donations? The two processes are different, and individuals can donate plasma more often and for $30-$100 per visit – a growing income stream for many Americans.
Jaworski and English found that when a plasma donation center opened near a blood donation center in the United States, there was a small but positive increase in blood donations.
“Rather than taking blood donors away, the plasma center made it so that there was just a tiny bit more blood donation in those cities than in comparable cities that did not have a plasma center,” he said.
Disseminating Knowledge More Broadly

In January, Jaworski launched the Georgetown Blood and Plasma Research Group to better collate and disseminate data about plasma, blood and bone marrow collections and promote interdisciplinary research.
He’s also a principal ethics member of United Plasma Action, which recently partnered with the United Nations Institute for Training and Research.
In June, he’ll receive the 2026 Plasma Hero Award from the Immune Deficiency Foundation, which honors individuals who work to ensure patients have access to the medications and therapies they need.
Ten years after beginning this venture, it’s still making Jaworski tick.

“There’s a little bit of this mystery detective trying to figure out where the data is. How much plasma did Finland collect last year? How do I figure that out?” he said. “There are the patients. That’s a lot of the passion. Then there’s also the fact that hardly anybody else is looking for this data, and there’s a lot of interest.
“Bioethicists sometimes disagree with me, and there are people in the Red Cross who disagree with me, and people who work in public blood collection centers who disagree with me. But I need to keep working on bridging that gap and helping them to see the other side of the issue.”
Jaworski also brings the topic into the classroom for his undergraduate and graduate students to untangle.
“When we talk about passion and purpose in the work that you do, I end with, ‘I hope you find your plasma — the thing that makes you really excited to get up and do work. It’s very exciting.’”